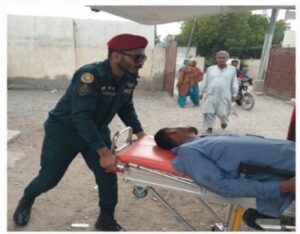
Government of Balochistan had approved an emergency response center project for coastal highway and released Rs. 707.00 million budgets to PPHI-B for establishment of six (6) ERCs on Makran Coastal Highway.
The project started in 2021. Human resource recruitment of Station Officer one (1) eighty-four (84) Cadets (including Emergency Medical Technicians 36, fire & Disaster Emergency Response Team Resource (11) & light Transport Vehicles Drivers (36) and forty-four supporting staff were completed. Technical Cadets were sent to Emergency Service Academy Punjab Lahore (1122) for six (6) months training. Training was completed in November, 5th, 2022. After completion of training cadets were deployed at 1122 MERC Balochistan for further capacity building and to provide rescue services to the people of Balochistan. ERC cadets were sent to JPMC for a 15 days training in two batch starting from 5th March, 2023 to 20th March, 2023 and 21st March, 2023 to 4th April, 2023.
Consultancy services were hired through NIT to work out complete design and maps for the proposed centers alongside resident engineer supervision during ongoing civil works at sites. Three sites Liyari, Phore and Rasmallan in District Lasbela and three sites Basol Ormara, Pasni Zeropoint and Nalaint in District Gwadar were established. Four (4) ERC sites of District Lasbela and Gwadar were tendered for construction and awarded to bidders. Construction works including Phase-B are under progress and near to completion.
The Procurement of six (6) Ambulance including six (6) rescue bike has been also completed in January 25th, 2023 and handed over to the vender for Fabrication, after fabrication ambulances were deployed at field on 20th July, 2023. Basic necessary equipment and medicine purchased and provided to all ERC sites, while for other major equipment and furniture tender process is under progress and procurement is expected to be complete before 1st June, 2024.
Detail of Emergency Response Canters started to provide services on Coastal Highway
- ERC Liyari District Lasbela in March, 2023
- ERC Rasmallan District Lasbela in March, 2023
- ERC Pasni District Gwadar in May, 2023
- ERC Ormara District Gwadar in May, 2023
- ERC Phore District Lasbela in July, 2023
- ERC Nalent District Gwadar in July, 2023
Detail of Emergency Response Centres has provided services on Coastal Highway March, 2023 to 31st December.
S# | ERC Centre | Highway | No. of Incident Responded | No. of Injured treated | No. of Death recorded |
1 | ERC Liyari | N-10 | 92 | 127 | 2 |
2 | ERC Phore | N-10 | 96 | 165 | 6 |
3 | ERC Rasmallan | N-10 | 62 | 74 | 1 |
4 | ERC Ormara | N-10 | 48 | 108 | 4 |
5 | ERC Pasni Zeropoint | N-10 | 46 | 85 | 10 |
6 | ERC Nalaint | N-10 | 22 | 25 | 1 |
Total | 366 | 584 | 24 | ||